

Understanding Urinary Incontinence
Urinary incontinence refers to the involuntary leakage of urine, which can vary in severity from occasional light leaks to complete loss of bladder control. It can significantly impact daily life, causing embarrassment, anxiety, and a reduced quality of life for those affected.
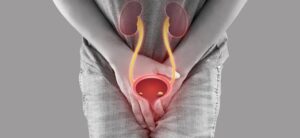
Types of Urinary Incontinence
There are several types of urinary incontinence, each with its own causes and symptoms:
1. Stress Incontinence
Stress incontinence occurs when there is pressure on the bladder, such as during coughing, sneezing, laughing, orexercising. It is often due to weakened pelvic floor muscles, which support the bladder and urethra.
2. Urge Incontinence
Urge incontinence, also known as overactive bladder, involves a sudden, intense urge to urinate followed by an involuntary loss of urine. It can be caused by neurological issues, bladder irritation, or other medical conditions.
3. Overflow Incontinence
Overflow incontinence happens when the bladder does not empty properly, causing it to overflow. This can occur due to a blockage or obstruction in the bladder or urethra, or weak bladder muscles.
4. Functional Incontinence
Functional incontinence occurs when physical or cognitive impairments prevent someone from reaching the toilet in
time. It is common in elderly individuals with mobility issues or dementia.
Causes of Urinary Incontinence
Understanding the underlying causes of urinary incontinence is crucial for effective management. Common causes
include:
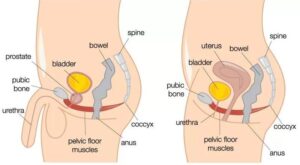
Diagnosing Urinary Incontinence
Proper diagnosis is essential to determine the type and cause of urinary incontinence. It typically involves:
Treatment Options
Effective management of urinary incontinence depends on its type, severity, and underlying causes. Treatment options
include:
Lifestyle Modifications
Medications
Surgical Interventions
Advanced and Latest Treatment
Why Choose SIS Therapy?
SIS therapy stands out due to its non-surgical approach and high success rates in treating urinary incontinence. By targeting and strengthening pelvic floor muscles through electromagnetic stimulation, SIS therapy offers:

Conclusion: Discover the Best Treatment for Urinary Incontinence with Super Inductive System (SIS) Therapy
Urinary incontinence can significantly impact daily life, but with advancements like Super Inductive System (SIS) therapy, effective treatment is now within reach. SIS therapy offers a non-invasive solution that strengthens pelvic floor muscles, providing lasting relief from incontinence symptoms. As you consider your options for managing urinary incontinence, it’s crucial to understand the benefits of SIS therapy in improving your quality of life.
FAQs About Managing Urinary Incontinence with SIS
1. How does SIS differ from traditional muscle stimulation therapies? SIS utilizes advanced technology for deeper and more effective muscle stimulation compared to traditional methods.
2. Is SIS suitable for all types of urinary incontinence? SIS is particularly effective for stress incontinence and overactive bladder, but its suitability should be determined by a healthcare professional.
3. Are there any age restrictions for SIS treatment? Generally, there are no specific age restrictions, but individual health assessments are necessary to determine suitability.
4. Can SIS treatment be combined with other therapies? Depending on the patient’s condition, SIS treatment can sometimes be complemented by other therapies as part of a comprehensive treatment plan.
5. How long does it take to see results with SIS? While results may vary, many patients report improvement within a few weeks of starting SIS treatment.
