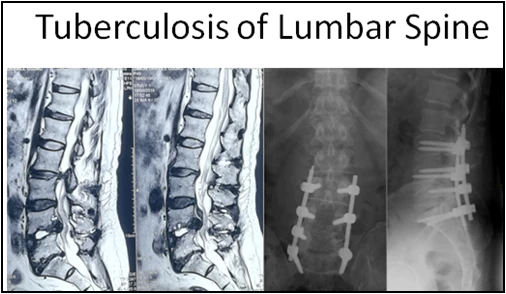
Popularly known as Pott’s disease, spine tuberculosis is a spinal infection which results in osteomyelitis, kyphotic deformity and spinal mechanical instability.
While in the absence of neurological defects, it is treated with bracing and anti-tuberculosis antibiotics, in the presence of the same, surgical management is required to improve recovery time of spine TB patients.
In early stages, the infection begins in metaphysics of the vertebral body, spreads under anterior longitudinal ligament, develops to contiguous multilevel involvement, skip lesion or non contiguous segments and paraspinal abscess formation which is usually anterior.
Speaking about chronic infection or severe kyphosis, mean deformity in non-operative cases could be 15 degrees while in few patients’ deformity is greater than 60 degrees. Since it is diagnosed late, in severe kyphosis have granulomatous spinal infections. While kyphosis is static in adults after healing, it progresses 40 percent in children owing to growth spurt.
Delay in diagnosing the disease or insufficient management increases the complications leading to spinal cord decompression and spinal deformity and delays recovery time of spine TB patients which are characterized by Gibbus deformity, pain and palpable masses.
Table of Contents
Spine TB is usually experienced by pain in site of infection, which is accompanied by fever, night sweat, weight loss, loss of appetite and with prominence of vertebral defect, localized deformity might be observed.
Spine TB is different from pulmonary TB. Multiple mycobacterial populations with varying growth kinetics and metabolic attributes are strictly aerobes and thrive in oxygen rich areas like lungs. Higher inclination of multibacillary involvement is present.
In contained osseous tissue, organism multiplies but not in the same magnum. In spine TB, the areas are paucibacillary with dormant mycobacteria which are harder to be destroyed and chemotherapy is obsolete in challenging its viability.
The treatment of spinal TB is challenging where decision making is complicated owing to the lack of evidence and guidelines which in sufficiency could result in optimal treatment and management strategies.
Normally immobilization enabled by body casts and healthy diet are advocated as treatment methods. Anti TB drugs are not instantly employed since they have risks such as instability and progression of neurological deficit (whose progress insists surgery).
The anti TB therapy extends from 9 to 18 months or more which is a multi perspective burden to the patients given the social, economic and lifestyle setbacks that the patient has to go through.
Patients are advised to take bed rest for 6 to 8 weeks till pain decreases and if neurological deficit appears three weeks after therapy, surgical intervention is proposed.
Surgical options like anterior spinal fusion, anterior posterior spinal fusion, posterior spinal fusion and posterior fusion followed by anterior fusion are available. However lack of information on safety, neurological results and complication rates pertaining to surgical intervention keeps indication for surgical intervention unclear.
During treatment, patients may experience loss of appetite, nausea and pain in joints. Mild painkillers such as aspirin and paracetamol are consumed to handle the pain.
Reportedly, after surgery patients are immobilized with braces for minimum three months and continued with chemotherapy along with steroids like isoniazid, rifampin and ethambutol for minimum one year.
Neurological recovery is good after surgery in child and adolescent patients. Most children with nerve dysfunction recover between 2 to 36 months. The neural functional recovery rate is reportedly between 76 to 91 per cent.
Post surgery patients are offered physiotherapy treatment for at least a month.
After 4 to 6 weeks of chemotherapy, ESR and C-reactive protein decreases. It is to be noted that ESR and CRP are reliable parameter in assessing response to spine TB treatment. Negative CRP is associated with poor results.
However, suggestions to combine hyperbaric oxygen therapy with anti TB treatment to decrease treatment duration require more studies to attain support.